What exactly does “storiform” mean?
Do you know what a “storiform” pattern is? Yeah, neither did I when I was a medical student. However, that term did get thrown around in pathology lectures a lot, without any description or definition. There are lots of terms like this – so I’m gonna just go ahead and create a new category called:
Words Pathologists Use In Lecture As If You Know What They Mean.
I think it’s important to pause and define these terms, because otherwise this is what happens: given the sheer volume of stuff you’re supposed to learn, and the minimal amount of time you have to accomplish this task, you’re not going to look up every word you have a nagging doubt about. You’re going to infer the meaning from whatever was said in lecture, and wind up with a fuzzy and probably incorrect definition. And then someone will ask you about it on rounds, and it will be frustrating.
SO. We’ll start with “storiform” today – and I’ll keep adding posts about terms in this category as I run across them. Please email me if you find a word like this! Then we’ll wind up with a nice glossary of these formerly-unexplained terms, and you’ll look like the star you are when one of these terms comes up on rounds.
First, a little Latin
Storiform comes from the Latin storea (woven mat) and formis (form, or pattern) – so technically, storiform means “having the pattern of a woven mat.” When we use “storiform” in pathology, though, it has a more specific meaning. It refers to a tumor pattern consisting of spindle cells in a pinwheel-shaped arrangement (radiating out from a central core).
What does it look like?
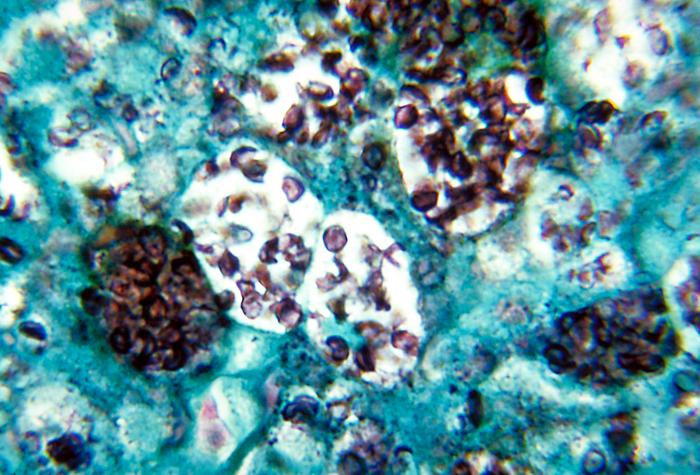
Sooo…what does a pinwheel-shaped arrangement of spindle cells look like under the microscope? Let’s try looking at an un-marked slide first, just to see if you can find pinwheels on your own. Here’s an image (below, right) of a skin lesion called dermatofibrosarcoma protuberans (DFSP), which is known for its storiform pattern. Take a look and see if you can find areas where the tumor cells are arranged in a pinwheel-shaped fashion. Then scroll down to see a labeled image.


Ready to see the labeled image? Okay, scroll down….
.
.
.
.
.
.
.
.
Keep going…
.
.
.
Here’s the same image, faded out a bit so you can see the pinwheel-shaped areas outlined in black:

Okay, they’re not perfectly symmetrical pinwheels, but they do look pinwheel-ish, with tumor cells radiating out from a central core region.
One last thing, now that we’ve got the pinwheels down…if you go back and look at the unmarked image again, you might be able to imagine that the cells are arranged like a woven mat, like the Latin term suggests.
I hope you feel comfortable with “storiform” now. That’s one less undefined term!










Recent Comments