The first thing I think of when I hear “granuloma” is the Knack song My Sharona. It just fits so nicely in there, right where My Sharona would be…”Come a little closer, close enough to look at my granuloma.” Okay, it doesn’t make any sense, but maybe someone will come up with some nice memory device based on the song.
Silliness aside, you really need to know a few things about granulomas. There are a limited number of things that cause them – so when you see one, that narrows down your differential to a reasonably short list.
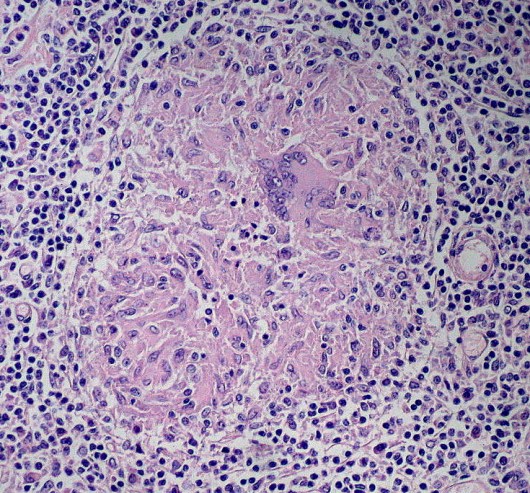
Granulomas are part of a special kind of chronic inflammation called, you guessed it, granulomatous inflammation. They represent the body’s attempt to contain a foreign agent that it can’t easily get rid of – like Mycobacterium tuberculosis, or talc. Histologically, they consist of a bunch of “epithelioid” macrophages (big, pink, activated macrophages that look like epithelial cells) surrounded by a collar of lymphocytes (and sometimes plasma cells). Sometimes these epithelioid macrophages fuse together, forming giant cells, with 20 or more nuclei inside (check out the giant cell in the granuloma above).
There are basically two kinds of granulomas: foreign body granulomas (formed in response to inert foreign objects, like talc or sutures) and immune granulomas (formed in response to any of a number of agents, like Mycobacterium tuberculosis or Treponema pallidum. Foreign body granulomas have the epithelioid macrophages described above, and sometimes you can see the foreign material (try using the polarizer and looking in the middle of the granuloma – foreign material is often refractile).
Immune granulomas can have a few different appearances, depending on their cause. Here’s a summary:
1. Tuberculosis. Granulomas in TB are sometimes called tubercles. They are caseating, meaning they are “cheesy” in gross appearance. Histologically, there is a bunch of amorphous, granular, necrotic debris in the center of the granuloma. You should see some acid-fast bacilli in there too.
2. Leprosy. These granulomas are non-caseating, and an acid-fast stain should reveal bacilli.
3. Syphilis. Granulomas in syphilis are called gummas; they have central necrosis (but not really caseating, because you can still see cell outlines) and a plasma cell infiltrate.
4. Cat-scratch disease. These granulomas may be stellate in appearance. They contain neutrophils and some granular debris, but giant cells are rare.
5. Sarcoidosis. Granulomas in sarcoidosis are non-caseating, with a lot of activated macrophages.
6. Crohn disease. Sometimes you see non-caseating granulomas in the intestinal wall in patients with Crohn disease.
That’s it in a nutshell. Now if I could just get that song out of my head…








You can try with the Deep Purple: one pain drives out another!
Best regards.
Nice description.
good description
Thanks great summary for my USMLE.
Really helpful!
Great! Thanks!
According to the London school of medicine, they are also caused by fungi. Aspergillis, which is a common mold found in many water damaged buildings, can cause granulomas. Not enough focus in fungi in American medical schools. It’s a shame as they cause all kinds of havoc. You may want to add fungi to your list 🙂
Thanks, Jennifer – you’re absolutely right: fungi can cause granulomas too. I tend to go by Robbins for a nice summary when it comes to things like “what causes granulomas?” – and it lists the following as the top causes: tuberculosis (the prototype), sarcoidosis, cat-scratch disease, lymphogranuloma inguinale, leprosy, brucellosis, syphilis, some mycotic infections, berylliosis, reactions of irritant lipids, and some autoimmune diseases. So yes – fungal (mycotic) infections are definitely on the list. Thanks for your comment!
Hey Dr. Krafts–thanks for this! have you ever happened to come across–or made yourself–a good table that lists and compares all or most types of caseating v noncaseating granulomas?
Hi Ben –
Yes – Robbins has a little table, Table 2-8 on page 73 (edition 8e), which lists the type of granulomas you see in TB (caseating), leprosy(non-caseating), syphilis (gumma), cat-scratch disease (stellate), sarcoidosis (non-caseating), and Crohn disease (non-caseating). There’s more histologic info listed in there too.
Thank you! I’ve been trying to figure out what a granuloma was since August, and I finally get it!
Great!! So glad to help.
Very helpful,thanku
Thanku,very helpful
Thanks Dr Krafts for this simple and insightful description.